Achilles Tendonitis

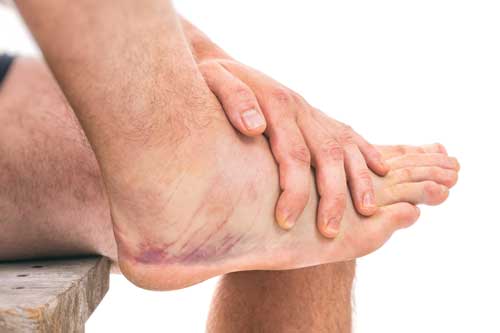
Achilles tendonitis is a painful and often debilitating inflammation of the Achilles tendon (heel cord). The Achilles tendon is the largest and strongest tendon in the body. It is located in the back of the lower leg, attached to the heel bone (calcaneus), and connects the leg muscles to the foot.
The Achilles tendon gives us the ability to rise up on our toes, facilitating the act of walking, and Achilles tendonitis can make walking difficult almost impossible.
There are the three stages of tendon inflammation:
- Peritenonitis
- Tendinosis
- Peritenonitis with tendinosis
Poorly conditioned athletes are at the highest risk of developing Achilles tendonitis. Participating in activities that involve sudden stops and starts and repetitive jumping (e.g. basketball, tennis, dancing) increased the risk for the condition. It often develops following sudden changes in activity level, training on poor surfaces, or wearing inappropriate footwear.
Achilles tendonitis may be caused by a single incident of overstressing the tendon, or it may result from a series of stresses that produce small tears over time (overuse). Patients who develop arthritis in the heel have an increased risk for developing Achilles tendonitis. This occurs more often in people who are middle aged and older.